Needles and sharps instruments are essential to dentistry practice which is why sharps injury rates are a huge concern for dentists.
A study of Needlestick and Sharps Injury (NSI) cases reported by a university hospital in Taiwan between 2009 and 2011 showed that the annual incidence of sharps injuries was 8.19% among all dental workers. Those with less experience, for example interns, had a higher percentage of Needlestick and Sharps Injury incidences at 21.28% per year. Other NSI incidences per person-year: 7.50% for residents, and 6.77% for nursing staffs (1). This does not account the numbers of sharps injuries that go unreported.
In the study, a total of 56 injuries were reported by the university. In 16 of the 56 cases, the injury was caused by cutting instruments, such as periodontal curettes, surgical scalpels, and scissors (1).

What can we expect if we get injured?
Sharps injuries have a number of serious consequences for individuals. In the best case, a sharps cut would just require time off work as well as blood tests. . In the worst scenario, you are risking surgery, a blood-borne infection, or costly rehabilitation for you and your practice. There are infection risks of Hepatitis B (HBV), hepatitis C (HCV), and human immunodeficiency virus (HIV) transmission (4).
Do sharps regulations work?
A 2017 needlestick injury survey by the British Association of Dental Nurses (BADN), showed that 48% of respondents had received a needlestick and sharps injury at work, and 58% of which had experienced more than one incident(3). Comparisons to the 2014 survey indicate a decrease in NSI cases after 3 years of sharps regulations were implemented.
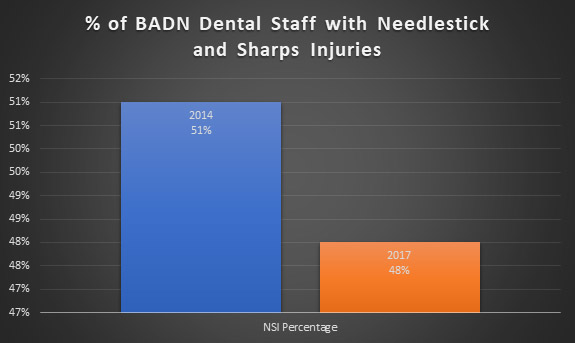
Regulations are established to protect the people and provide essential safeguards for the community. An effective sharps safety program is shown to have reduced injuries by as much as 80% (5).
Reducing injuries by implementing a sharps safety program
To manage and prevent the occupational risks of scalpel injuries, dentists and dental clinics should consider developing and implementing a combination of controls, following the guidelines stated by Queensland Health as follows (6):
An effective sharps safety program includes three core elements which should be implemented simultaneously:
-
- engineering controls, such as:
- use of sharps disposal systems that conform to Australian Standards (AS4031 or AS/NZS 4261)
- sharps removal systems (e.g. scalpel blade removers)
- work practice controls, such as:
- availability of point of use sharps containers
- establishing a responsibility practice – the person who generates the sharp is responsible for the safe disposal of the sharp
- training, including:
- on induction and annual education as it should not be assumed that new staff are familiar with specific devices used or policies and procedures related to sharps safety
- introduction of a new device
- engineering controls, such as:

In the U.S., OSHA’s Bloodborne Pathogens Standard requires the implementation of an exposure control plan to use engineering and work practice controls, personal protective clothing and equipment, and employee training to minimise the risks of scalpel hazards (7).
Hierarchy of Controls
The Hierarchy of Controls is a very effective method for managing hazards in the workplace and should be followed to prevent sharps injuries to healthcare workers. This approach differs from previous behaviour-based safety approaches, by addressing the initial sources of hazards experienced by workers. The hierarchy establishes five levels of hazard control measures, which are prioritised according to their effectiveness. These levels are:
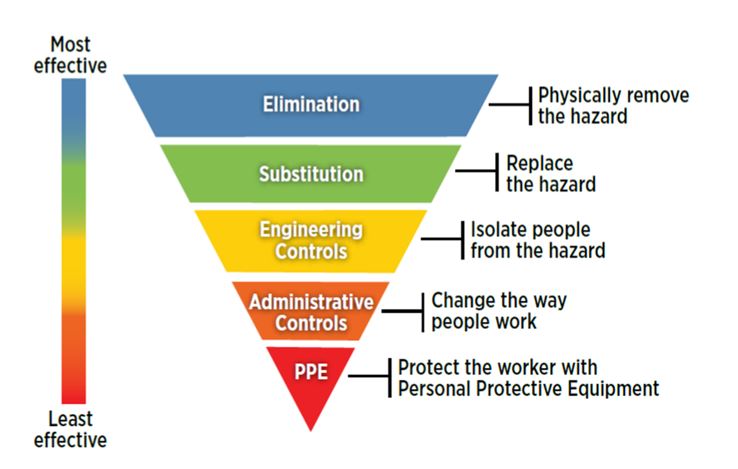
Both Australia’s Queensland Health and U.S.’ OSHA recommend using engineering controls. Qlicksmart’s BladeFLASK and BladeFlask EVO are safety-engineered devices which can help your dental practice/clinic prevent sharps injuries and comply with the requirements. Implementing engineering controls enhances the safety of traditional devices. Specifically, engineering controls incorporate safety mechanisms designed to either isolate or remove the hazard from the environment. It is therefore most useful when alternative instruments or procedures are not adequate or appropriate.

Qlicksmart single-handed scalpel blade removers
Single handed blade removers like those pioneered by Qlicksmart can be seamlessly integrated into a dental clinic’s safety program by:
-
- Use of a scalpel blade removal system mounted in several stationary points within the dental surgery increasing its accessibility – scalpel blade removal can be completed at point of use.
- Automatic containment of used scalpel blades ensures that all personnel are protected from injury.
Qlicksmart’s BladeFlask EVO is able to singlehandedly remove blades from scalpel handles often used in oral and dental surgery including circular and Barron handles. Even the Bard-Parker 3LA bent handle used specifically with dental procedures can ONLY be used the BladeFlask EVO. This makes the BladeFlask EVO Scalpel Blade Remover the perfect addition to your dental surgical practice.
To find out more on how to keep your dental practice safe from scalpel cuts, send us an email at hello@copyqlicksmart.kinsta.cloud.
References
1. Lee, Jang-Jaer & Kok, Sang-Heng & Cheng, Shih-Jung & Lin, LD & Lin, C.-S. (2014). Needlestick and sharps injuries among dental healthcare workers at a university hospital. Journal of the Formosan Medical Association. 113. 227–233. 10.1016/j.jfma.2012.05.009.
2. Fareedi Mukram Ali, Ashok Patil, Prasant M.C, Safiya Tahasildar, Kishor Patil. “Needle Stick injuries in Dental Clinics: A Review”. Journal of Evolution of Medical and Dental Sciences 2014; Vol. 3, Issue 02, January 13; Page: 374-378, DOI:10.14260/jemds/2014/1836
3. British Association of Dental Nurses. BADN Initial Medical Needlestick Injury Survey 2017 Report
4. Taylor, D. C., Matson, A. P., Gibson, S. D., Glover, S., Bartis, J., Ruch, D. S., & Richardson, W. J. (2018). Ulnar Nerve Transection in an Orthopaedic Surgeon Sustained During Surgery: A Case Report and Commentary. The Journal of bone and joint surgery. American volume, 100(1), e2. http://doi.org/10.2106/JBJS.17.00226
5. Visser L. (2006). Toronto hospital reduces sharps injuries by 80%, eliminates blood collection injuries. A case study: Toronto East General Hospital pioneers healthcare worker safety. Healthcare quarterly (Toronto, Ont.), 9(1), 68–4. http://doi.org/10.12927/hcq..17907
6. Queensland Health. (2017). Developing a sharps safety program. http://www.health.qld.gov.au/clinical-practice/guidelines-procedures/diseases-infection/infection-prevention/standard-precautions/sharps-safety/sharp-safety-program
7. OSHA Bloodborne Pathogens and Needlestick Prevention. http://www.osha.gov/bloodborne-pathogens